Food Sensitivity Testing: Your Guide to At-Home Kits and Clinic Options
Confused by food sensitivity testing? Learn the truth about at-home kits vs. clinical options for real answers & relief.

Why Understanding Food Sensitivity Testing Matters
Food sensitivity testing has become a multi-million dollar industry, promising answers to persistent health complaints. But not all tests are created equal.
Quick Answer: What You Need to Know About Food Sensitivity Testing
- Scientifically Validated Tests: Skin prick tests, blood IgE tests, and oral food challenges (for true IgE-mediated allergies only)
- Not Recommended: IgG antibody tests, hair analysis, kinesiology, electrodermal testing
- Best Diagnostic Approach: Medical history + elimination diet under professional supervision
- Key Fact: IgG antibodies indicate exposure to foods, not sensitivity or intolerance
- Professional Consensus: Major allergy organizations advise against IgG testing for food sensitivities
If you're dealing with bloating, fatigue, skin issues, or other persistent symptoms after eating, you've probably seen the promise of a simple test that can identify your "trigger foods." The market is flooded with at-home kits and clinic options, each claiming to open up the mystery of your discomfort.
Here's the challenge: navigating the confusion between legitimate medical testing and unproven methods that may lead you down the wrong path.
The numbers tell an important story. Approximately 12% of Americans have a confirmed food allergy or intolerance, while an estimated 23% of the world population may live with undiagnosed food sensitivities. With so many people searching for answers, it's no surprise that testing options have exploded—but not all of them are backed by science.
The stakes are real. Unnecessary food avoidance based on unreliable tests can lead to nutritional deficiencies, reduced quality of life, and increased anxiety. Meanwhile, true food allergies require accurate diagnosis and proper medical management to prevent potentially life-threatening reactions.
I'm Dr. Doug Jones, a board-certified immunologist who has spent over a decade helping patients steer complex immune challenges, including food sensitivities and allergies. Through my work at GAIN—Global Allergy Immune Network—I've seen how proper food sensitivity testing and diagnosis can transform lives, and how unproven methods can lead patients astray.

Food Allergy, Sensitivity, or Intolerance? Understanding the Key Differences
When we talk about adverse reactions to food, it's easy to get lost in the terminology. Are you experiencing a food allergy, a food sensitivity, or a food intolerance? While these terms are often used interchangeably, they represent distinct reactions within our bodies, each with its own set of symptoms and diagnostic approaches. Understanding these differences is the first crucial step in finding effective relief.
Let's break down the core distinctions:
| Criteria | Food Allergy | Food Sensitivity | Food Intolerance |
|---|---|---|---|
| Immune System Response | IgE-mediated (Type 1 hypersensitivity) | Non-IgE immune response, or other mechanisms (e.g., IgG) | No immune system involvement |
| Symptom Onset | Immediate (minutes to 2 hours) | Delayed (hours to days) | Delayed (hours) |
| Symptom Types | Hives, swelling, difficulty breathing, vomiting, anaphylaxis | Bloating, cramping, diarrhea, headaches, fatigue, skin issues, mood changes | Bloating, gas, diarrhea, stomach pain, nausea (digestive symptoms) |
| Diagnostic Method | Skin prick test, IgE blood test, oral food challenge | Elimination diet with reintroduction | Elimination diet, hydrogen breath test (e.g., lactose) |
Food Allergy
A true food allergy is a serious medical condition involving an immediate and specific immune system response. Our immune system mistakenly identifies a harmless food protein as a threat and produces immunoglobulin E (IgE) antibodies. When we then consume that food, these IgE antibodies trigger a rapid release of chemicals like histamine, leading to symptoms that can range from mild to life-threatening.
Symptoms of a food allergy can include itching, rash, hives, swelling, difficulty breathing or swallowing, vomiting, and in rare cases, anaphylaxis, which can be fatal. Approximately 12% of Americans have one or more food allergies or intolerances confirmed by a health professional. This is why diagnosing food allergies accurately is paramount; it's not just about comfort, but about safety.
Food Intolerance
Unlike an allergy, a food intolerance does not involve the immune system. Instead, it's a digestive system issue. Our bodies may lack the enzymes needed to properly break down certain foods, or we might be sensitive to specific chemicals or additives in food.
A classic example is lactose intolerance, where individuals lack sufficient lactase, the enzyme required to digest the sugar (lactose) found in dairy products. When undigested lactose reaches the large intestine, it ferments, causing symptoms like bloating, cramping, and diarrhea. While uncomfortable, food intolerances are generally not life-threatening.
Food Sensitivity
The term "food sensitivity" is often the most confusing because it's a bit of a catch-all. It's a non-specific term that can include any symptom perceived to be related to food. Food sensitivities typically involve a delayed reaction, with symptoms appearing hours or even days after consuming a trigger food. These reactions may involve the immune system (but not IgE antibodies in the way allergies do) or other biological mechanisms that are not fully understood.
Symptoms of food sensitivities are broad and can affect various body systems, including mood, appetite, skin, digestive health, and physical health. They might manifest as bloating, cramping, diarrhea, headaches, fatigue, brain fog, or skin issues like eczema. Because the symptoms are delayed and often non-specific, identifying trigger foods can feel like trying to catch smoke.
For a deeper dive into these distinctions, we encourage you to read our article on the difference between food intolerances, sensitivities, and allergies.
Clinically-Proven Methods for Diagnosing Food Reactions
When it comes to diagnosing reactions to food, we must prioritize methods that are scientifically validated and recommended by leading medical organizations. Guesswork and unproven tests can lead to unnecessary dietary restrictions, nutritional deficiencies, and prolonged suffering. Our goal is to be detectives, as Dr. Mark DeMeo, a gastroenterologist, aptly puts it: "Everybody that comes in the door has a different story. And so you start off trying to be a detective." This means a thorough, personalized, and evidence-based approach.
Scientifically Validated Allergy Tests
For true IgE-mediated food allergies, there are established, reliable diagnostic tools that a board-certified allergist will employ. These tests help us accurately identify the specific allergens triggering an immune response.
Skin Prick Test
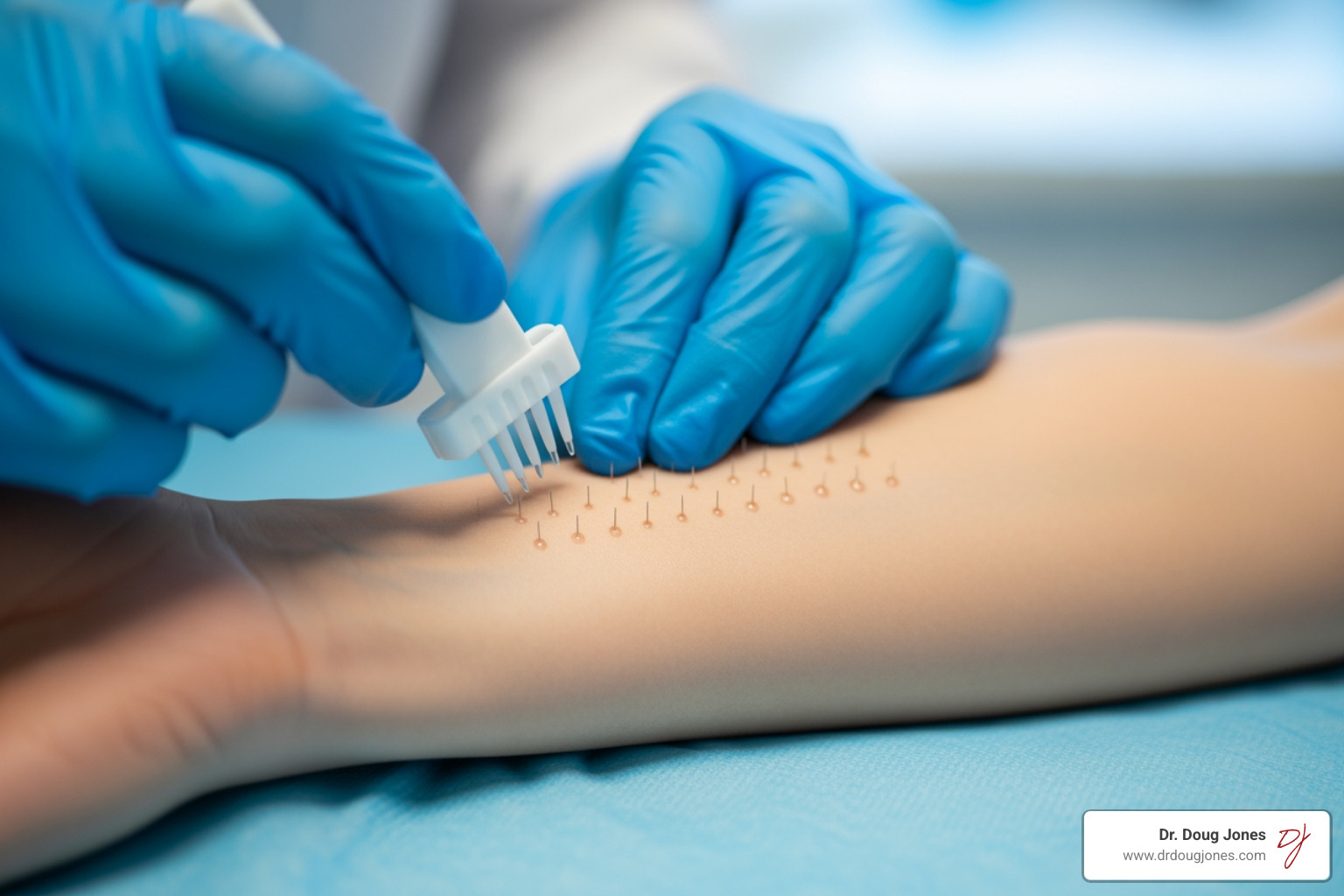
The skin prick test is a common and effective method for diagnosing IgE-mediated food allergies. During this test, a small drop of a liquid allergen extract is placed on your skin (usually the forearm or back), and the skin is lightly pricked or scratched, allowing the allergen to enter just beneath the surface. If you're allergic, a small, red, itchy bump (called a wheal) with a surrounding red area (flare) will typically appear within 15 to 30 minutes. The size of the wheal helps the allergist interpret the result, though it doesn't necessarily predict the severity of a future reaction. A positive result indicates sensitization, but not always a clinical allergy.
Blood Tests (IgE)
Blood tests for food allergies measure the amount of food-specific IgE antibodies in your blood. These tests, often called RAST or ImmunoCAP tests, provide a numerical value indicating your level of sensitization to a particular food. Results are usually available in one to two weeks. While helpful, a positive IgE blood test alone does not definitively diagnose a food allergy. It suggests a likelihood of allergy, but like skin prick tests, it needs to be interpreted in the context of your medical history and symptoms. A negative test, however, is often very good at ruling out an allergy.
Oral Food Challenge
Considered the "gold standard" for diagnosing food allergies, an oral food challenge involves carefully consuming increasing amounts of a suspected food under strict medical supervision. This test is performed in a clinic or hospital setting where medical staff can monitor for any reactions and intervene immediately if necessary. The oral food challenge is the most definitive way to confirm or rule out a food allergy, but it is not routinely performed due to its cost, time commitment, and the potential danger of inducing a severe allergic reaction. It's usually reserved for cases where other tests are inconclusive or when we suspect an allergy has been outgrown.
For more information on these diagnostic methods, visit our guide on Food Allergy Testing and Diagnosis from Dr. Doug Jones.
The Role of the Elimination Diet
While the above tests are crucial for food allergies, they aren't suitable for diagnosing food sensitivities or intolerances. For these, the elimination diet is our most powerful tool. In fact, major health organizations, including the British Dietetic Association, state that there are no validated tests to diagnose food sensitivity, and diagnosis relies on a detailed dietary history, elimination, and reintroduction.
An elimination diet is a systematic, supervised process where you temporarily remove suspected trigger foods from your diet for a period (typically several weeks) to see if your symptoms improve. If symptoms subside, foods are then reintroduced one by one, in a controlled manner, to identify which specific foods provoke a reaction.

This process requires meticulous record-keeping, often involving a food diary, to track everything you eat and any symptoms you experience. It's vital that an elimination diet is undertaken with the guidance of a healthcare professional, such as a registered dietitian, to ensure nutritional adequacy and proper symptom interpretation. Importantly, an elimination diet should never be used for suspected food allergies, as reintroducing an allergen could trigger a dangerous reaction.
A Critical Look at At-Home Food Sensitivity Testing
The allure of quick answers from the comfort of your home is powerful. Food sensitivity testing has become a booming market, with countless direct-to-consumer tests promising to identify the culprits behind your discomfort. These kits often market themselves as the key to open uping a wide range of symptoms, from bloating and fatigue to migraines and skin issues. They often come with impressive-looking charts and personalized elimination plans. However, we must approach these claims with a healthy dose of skepticism.
Why IgG Food Sensitivity Testing is Not Recommended
Many at-home food sensitivity testing kits primarily measure immunoglobulin G (IgG) antibodies to various foods. While this might sound scientific, here's the crucial insight: IgG antibodies are a normal, healthy response to food exposure. They are memory antibodies, indicating that our immune system has encountered a particular food. Higher levels of food-specific IgG often simply mean that we eat that food regularly.
Consider this: when children outgrow food allergies, their IgE levels decrease, while their IgG levels to that food actually increase, signaling developing tolerance, not sensitivity. This is why leading allergy professional organizations, including the American Academy of Allergy, Asthma & Immunology (AAAAI) and the European Academy of Allergy and Clinical Immunology (EAACI), specifically recommend against using IgG tests for any purpose in diagnosing food allergies or sensitivities. The British Dietetic Association (BDA) also advises avoiding IgG blood tests, stating there is no convincing scientific evidence to support their use.
Relying on IgG food sensitivity testing can lead to significant problems:
- False Positives: Since IgG antibodies are a normal response to food, these tests frequently flag foods you regularly eat as "sensitive," even if they cause no symptoms. This can lead to unnecessary food avoidance.
- Unnecessary Food Avoidance: Eliminating healthy, nutrient-rich foods based on unreliable tests can lead to nutritional deficiencies, particularly if major food groups are cut out. It can also create an unhealthy relationship with food and reduce quality of life.
- Lack of Scientific Validation: There are simply no validated tests to diagnose food sensitivity using IgG antibodies. The presence of IgG antibodies does not correlate with clinical symptoms of food sensitivity.
For a comprehensive understanding of why these tests are problematic, we highly recommend reading this scientific review of blood testing for food sensitivity and our own article on the myths surrounding food sensitivity tests.
Other Unproven Food Sensitivity Testing Methods
Beyond IgG antibody tests, a host of other unproven methods are marketed for food sensitivity testing. These include:
- Kinesiology: Also known as muscle testing, this involves assessing muscle strength changes when in contact with a food.
- Hair analysis: Claims to detect sensitivities by analyzing hair samples.
- Electrodermal testing (Vega test): Uses an electrical device to measure changes in electrical resistance when a food is introduced.
- ATCAT (Antigen Leucocyte Cellular Antibody Test): Involves observing changes in white blood cells when exposed to food extracts.
- Pulse testing: Monitors changes in pulse rate after consuming a food.
- Provocation-Neutralization testing: Involves injecting small amounts of suspected allergens and observing reactions.
The consensus among medical professionals is clear: these methods lack scientific validation and are not reliable for diagnosing food hypersensitivity. The British Dietetic Association (BDA) provides a helpful factsheet on unproven tests, reiterating that they are no better than chance and should be avoided.
Making an Informed Decision: How to Get Real Answers
In a world full of conflicting health information, how can we differentiate between reliable medical advice and clever marketing claims? The key is critical thinking and understanding that if something sounds "too good to be true," it probably is. Especially exercise caution if the medical information is provided by the same company selling a service. This represents a clear conflict of interest.
The consequences of misdiagnosis based on unproven tests can be significant:
- Nutritional Deficiencies: Unnecessary food avoidance, particularly of major food groups, can lead to inadequate intake of essential vitamins and minerals. The Journal of the Canadian Medical Association warns that removing essential nutrients like iron and B12 from a child's diet based on unproven tests can be detrimental.
- Reduced Quality of Life: Constantly worrying about what to eat, adhering to overly restrictive diets, and the social isolation that can come with it can severely impact your overall well-being.
- Increased Anxiety: The constant search for answers, the fear of "trigger" foods, and the frustration of ineffective treatments can heighten stress and anxiety, especially for parents of children with suspected food issues.
- Delayed Proper Diagnosis: Focusing on unproven methods can delay seeking appropriate medical care for conditions that do have validated diagnostic and treatment pathways.
Where to Seek a Reliable Diagnosis
If you suspect you have a food allergy, sensitivity, or intolerance, your path to lasting relief should always begin with reliable, evidence-based medical guidance.
- Start with Your Primary Care Provider: Your family doctor is your first point of contact. They can take a detailed medical history, discuss your symptoms, and help you determine the most appropriate next steps, including referrals to specialists.
- Consult a Board-Certified Allergist/Immunologist: For suspected food allergies (IgE-mediated reactions), an allergist/immunologist is the expert. They specialize in diagnosing and managing allergic conditions using scientifically validated tests like skin prick tests, IgE blood tests, and oral food challenges. As Dr. Doug Jones, a board-certified immunologist, we specialize in redefining complex immune challenges, offering personalized care and education.
- Work with a Registered Dietitian: For suspected food sensitivities or intolerances, a registered dietitian is invaluable. They can guide you through a supervised elimination diet, helping you identify trigger foods while ensuring you maintain a nutritionally complete and balanced diet. They are also experts in developing practical, sustainable eating plans.
Finding answers is often like detective work, as Dr. DeMeo noted. It requires careful history-taking, thoughtful investigation, and a personalized approach custom to your unique story. We are committed to empowering individuals with lasting relief through personalized care and education, guiding you away from misleading claims and toward effective solutions.
Conclusion: Your Path to Lasting Relief
Navigating food sensitivity testing can feel overwhelming, but we hope this guide has clarified the crucial distinctions between allergies, sensitivities, and intolerances, and highlighted the importance of evidence-based diagnostics.
The key takeaway is this: ditch the guesswork and prioritize scientifically validated methods. Unproven tests, particularly those measuring IgG antibodies, are misleading and can lead to unnecessary food avoidance, nutritional deficiencies, and heightened anxiety without providing real answers.
Your health journey deserves accurate information and professional guidance. As a board-certified immunologist, Dr. Doug Jones and our team are dedicated to providing expert, personalized care that redefines complex immune challenges. We empower individuals with lasting relief through personalized care and education, helping you understand your body and make informed choices.
Don't let marketing claims dictate your health decisions. Seek out qualified medical professionals who can offer reliable diagnosis and management strategies. When you understand your immune system and how it interacts with food, you take a powerful step towards true well-being.
